 Horaizon Orthopedic Implants
Horaizon Orthopedic Implants
 Horaizon Orthopedic Implants
Horaizon Orthopedic Implants
Hip fractures pose significant health challenges, particularly in the elderly population. According to the World Health Organization, over 1.6 million hip fractures occur annually worldwide, with an expected increase over the next decades. Effective surgical interventions are crucial to restore mobility and reduce complications. Trochanteric Fixation Nails are increasingly recognized as a reliable option for stabilizing these fractures.
Dr. Emily Stone, a leading expert in orthopedic surgery, emphasizes, “Using Trochanteric Fixation Nails can greatly enhance recovery outcomes for patients with hip fractures.” These nails provide stable fixation, allowing for early weight-bearing and rehabilitation. However, challenges remain. The surgical technique requires precise placement, and not all patients are ideal candidates. Improper alignment can lead to complications.
While the benefits are clear, potential pitfalls should not be overlooked. Close monitoring post-surgery is essential. Research indicates that revision rates can vary significantly, depending on the surgical technique used. Therefore, a thorough understanding of Trochanteric Fixation Nails and their application is vital for surgeons aiming to improve patient outcomes in hip fracture management.
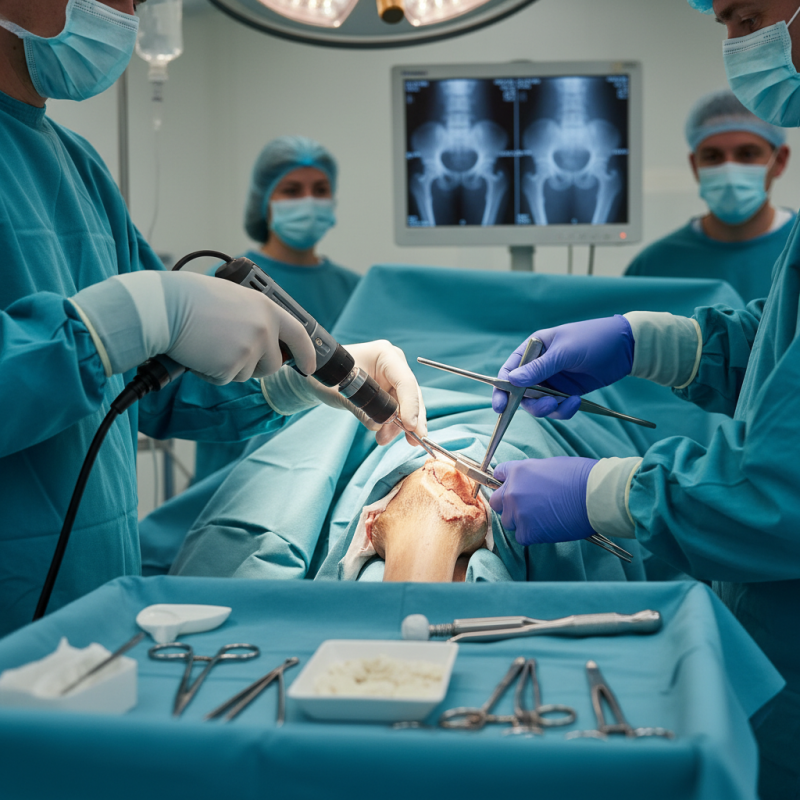
Trochanteric fixation nails are crucial for hip surgeries. They provide stability in complex fractures. Understanding their anatomy is vital. The design includes a long nail and locking screws. These components work together to ensure proper alignment of the bone fragments.
During surgery, surgeons insert the nail through the greater trochanter. Precision is essential for successful outcomes. The locking screws are then placed to secure the nail in position. This method helps patients regain mobility faster. However, improper placement can lead to complications. Surgeons must continually refine their techniques to avoid these issues.
Each case is unique. Some patients experience varying levels of pain post-surgery. Observing these differences can provide insights into improvements. Regular follow-ups are necessary for monitoring recovery. Adjustments may be needed based on individual healing rates. This reflects the ongoing learning process in surgical practice.
Trochanteric fixation nails provide a reliable solution for specific hip fractures. These nails are particularly indicated for intertrochanteric and subtrochanteric fractures. Patients with unstable or complex fractures often benefit the most. The surgical procedure can stabilize fractures by allowing for early mobilization. This is crucial for recovery.
In some cases, surgeons may encounter difficulties. Mechanically unstable fractures might complicate the process. Proper assessment is vital before surgery. Identifying the right patient is key to positive outcomes. Surgeons need to consider factors like age and bone quality. Each patient's anatomy poses unique challenges that can affect the surgery's success.
Additionally, post-operative care must be emphasized. Patients may experience pain or discomfort. Long-term mobility issues can arise if not managed correctly. Careful monitoring and follow-up appointments are necessary. Reflection on each case can lead to improved techniques and outcomes in trochanteric fixation.
| Indications | Description | Patient Profile | Surgical Considerations |
|---|---|---|---|
| Intertrochanteric Fractures | Fractures located between the greater and lesser trochanters of the femur. | Typically in older patients or those with osteoporosis. | Assess for bone quality and alignment before surgery. |
| Subtrochanteric Fractures | Fractures that occur below the lesser trochanter. | Often associated with high-impact injuries. | Careful placement of the nail to avoid fracture displacement. |
| Femoral Neck Fractures | Fractures that occur in the neck of the femur. | Common in elderly patients, with risk of avascular necrosis. | Consider fracture type for optimal fixation strategy. |
| Pathological Fractures | Fractures resulting from underlying bone disease. | Patients with cancer or metabolic bone disease. | Additional imaging may be required to assess bone integrity. |
Trochanteric fixation nails are crucial in hip fracture surgeries. They provide stability and support, especially in the elderly population. Studies show that hip fractures are prevalent among those over 65, with an incidence rate of approximately 300 fractures per 100,000 individuals. This makes understanding the trochanteric nail insertion process essential for surgeons.
The procedure typically begins with patient positioning. The patient is placed supine on the operating table. Then, the surgical site is prepared and draped. A small, lateral incision near the greater trochanter allows access. The next step involves drilling a guide pin into the bone correctly. Accuracy is vital; misplacement can lead to complications. Once the pin is in place, the nail is inserted over it. Care must be taken to ensure proper alignment. Postoperative x-rays are required to confirm correct positioning.
While the technique is generally effective, surgeons sometimes face challenges. For example, fractures may be more complex than anticipated. In such cases, the stability of the fixation may not be ideal. Reports indicate that improper techniques correlate with a reoperation rate of about 10%. Continuous education and practice are essential to minimize errors. Understanding these nuances can improve outcomes significantly.
Post-operative care after hip fracture surgery is crucial for recovery. Patients usually need to stay in the hospital for a few days. During this time, monitoring vital signs is essential. Nurses often check blood pressure and oxygen levels. Pain management is also a key focus. Patients might receive medication to control discomfort. It’s vital to communicate any pain levels to healthcare providers.
Once home, rehabilitation begins. This often includes physical therapy sessions. Exercises focus on restoring strength and range of motion. Patients may struggle with daily activities. Simple tasks like dressing or bathing can feel daunting. Family support becomes indispensable during this phase. It's important to encourage independence while ensuring safety.
Regular follow-ups with the doctor are necessary. These appointments help assess healing and recovery progress. Patients should be aware of signs of complications, such as swelling or unusual pain. Seeking advice promptly can prevent major setbacks. It’s not uncommon for patients to feel frustrated during recovery. Patience is key as healing takes time.
Trochanteric fixation nails have become a popular choice for hip fracture surgeries. However, potential complications can arise during and after the procedure. One common issue is nail migration. This can result from improper placement or inadequate fixation. Surgeons must carefully assess alignment during surgery. Awareness of this complication is crucial.
Infection is another significant risk. Postoperative infections can complicate recovery. Proper sterilization techniques and postoperative care are vital to minimize this risk. Early recognition of infection symptoms can lead to better outcomes. Some patients may experience nonunion or delayed union of the fracture. This could require additional surgical interventions. Continuous monitoring during recovery is essential.
Furthermore, complications related to hardware can occur. Breakage of the fixation nail can lead to further surgery. Regular follow-ups and imaging studies can help in timely detection. Surgeons should discuss these risks with patients before the procedure. Managing expectations is key to patient satisfaction. Open communication about possible complications fosters better patient relationships.
: They are used in hip surgeries to stabilize complex fractures effectively.
Surgeons insert the nail through the greater trochanter following precise techniques to ensure alignment.
Misplacement can lead to issues like instability and prolonged recovery times, necessitating improved techniques.
Patients with unstable intertrochanteric and subtrochanteric fractures usually gain the most benefit from this procedure.
Proper evaluation helps identify suitable candidates and predict potential difficulties during the surgical process.
They assess age, bone quality, and the unique anatomy of each patient to determine the best approach.
Patients may experience varying levels of pain and discomfort, which requires careful monitoring and follow-up.
Regular follow-ups help monitor healing and address any complications or mobility issues that may arise.
Ongoing training helps surgeons refine their techniques and reduce the chances of complications.
Improper techniques during the procedure have been linked to a reoperation rate of around 10%.
Trochanteric fixation nails are specialized orthopedic devices used in hip fracture surgeries to stabilize and promote healing in femoral neck and intertrochanteric fractures. Understanding their design and appropriate indications is essential for ensuring optimal surgical outcomes. These nails are particularly indicated for patients with unstable hip fractures and those with significant risk factors for non-union.
The insertion of trochanteric fixation nails involves a step-by-step procedure that requires careful alignment and fixation to ensure proper stabilization of the fracture site. After surgery, adequate post-operative care and recovery protocols are critical for patient rehabilitation. Monitoring for potential complications such as infection or malunion is necessary, with specific management strategies in place to address these issues. Overall, the effective use of trochanteric fixation nails can significantly enhance recovery and restore mobility in patients with hip fractures.
